Coding telehealth visits12/18/2023  articulation, phonological process, apraxia, dysarthria) with evaluation of language comprehension and expression (eg. articulation, phonological process, apraxia, dysarthria)Įvaluation of speech sound production (eg. stuttering, cluttering)Įvaluation of speech sound production (eg. Treatment of speech, language, voice, communication, and/or auditory processing disorder groupĮvaluation of speech fluency (eg. Treatment of speech, language, voice, communication, and/or auditory processing disorder individual To access a printable billing code cheat sheet for SLP’s click here Telehealth Procedure Codes for Speech-Language Pathologists To access a printable billing code cheat sheet for OT’s click here Telehealth Procedure Codes for Occupational Therapists Orthotic management and training, 1st encounter  
To access a printable billing code cheat sheet for PT’s click hereĪvailable up through year in which PHE ends 
Telehealth Procedure Codes for Physical Therapists Some codes require a timeframe of contact between the patient and qualified healthcare professional not originating from a related assessment or service provided in the previous 7 days, within the next 24 hrs., or the soonest available appointment (marked with * in our charts). When billing: These services require an established relationship between provider and patient.Virtual Check-ins: A virtual service where the provider conducts synchronous or asynchronous assessments or communicates with the patient via “a broader range of communication methods.” Telephone and short telehealth check-ins with patients fall under this category.These visits are billed using standard CPT codes that are accepted by Medicare for telehealth services. When billing: These services are covered for the duration of the COVID-19 public health emergency (PHE) if the provider already has an established relationship with the patient.Medicare Telehealth Visits: When the therapist offers a virtual service where the provider cares for a patient over a live, synchronous video stream.E-Visits: When a provider communicates and conducts synchronous or asynchronous assessments on a patient, typically through an online portal.We recommend reviewing the full Medicare Telemedicine fact sheet prior to submitting claims. You may also hear the term “communication technology-based services” or CTBS, which constitutes brief services conducted over different types of technology.Įach type of service will have different billing requirements that must be met to be covered by Medicare. “Virtual services” is the umbrella term CMS uses for remote visits. Medicare Telehealth Terminology and Billing Guidelinesįirst, let’s define the three types of virtual services Medicare covers. So, we’ve compiled this handy Medicare cheat sheet for outpatient rehab therapists, breaking down telehealth and communication technology-based service (CTBS) procedure codes.Ĭurious to learn more about Medicare Telehealth compliance? Check out this webinar with compliance expert Nancy Beckley. But knowing what remote services are covered by Medicare is critical to building a successful program. Additionally, many commercial payers have different requirements.įor physical therapists, occupational therapists, and speech-language pathologists, telehealth and other virtual services can be an excellent adjunct to your practice. Please note that these regulations change often, and while we will do our best to stay current, we advise you to also reference the CMS’s Telehealth Services page for the most accurate information. 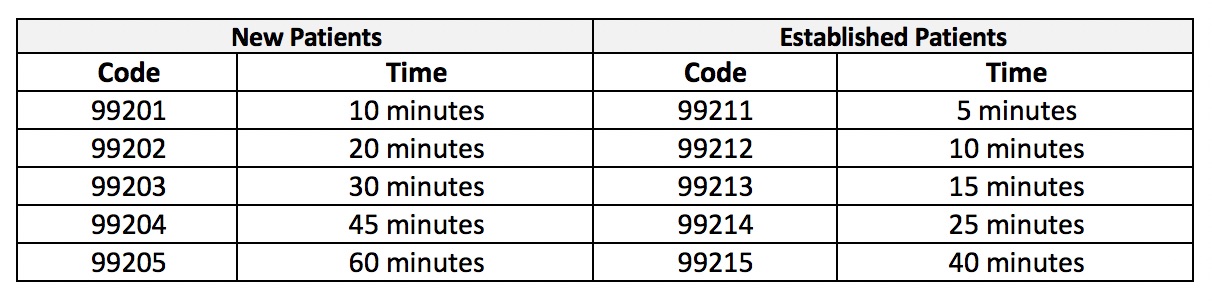
Editor’s note: The information contained in this article is current as of May 2021 and is based on CMS regulations. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
